Opioid overdoses kill tens of thousands of people annually in the United States and with the rise of drugs like oxycodone, heroin, and fentanyl, the problem doesn’t appear to be going away. In 2016 alone, those three drugs combined to kill more than 40,000 people and the number of fentanyl deaths has increased by more than 300% from 2014 to 2016.
With the emergence of opioids as a deadly drug, lawmakers and activists have been scrambling trying to find an answer to a problem that has caused the addiction of more than 2 million Americans and has impacted millions more. This has led to a number of legislative efforts to crackdown on the availability of the drugs and help treat those who have been affected by them.
One of the methods that first responders, medical professionals, and now regular citizens have begun to use to reduce the number of opioid overdose deaths is naloxone, a medication that can be used to reverse the effects of opioid overdoses. The availability of naloxone has become more widespread as politicians and emerge ncy services have come to understand the scope of the opioid epidemic and the impact that naloxone can have on it.
States like Oklahoma have passed laws to make the medication more readily available to all people while also fighting to make prescription opioids less widespread. For Oklahoma, a state that has one of the highest prescribing rates in the country, being ready for opioid overdoses when they will inevitably occur is key to staying ahead and saving lives.
What is Naloxone?
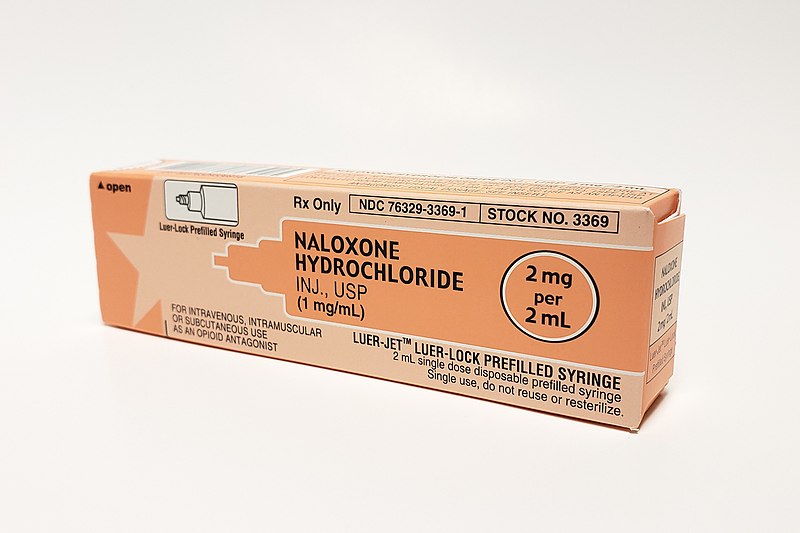
Naloxone is a medication designed to reverse an opioid overdose. It is an opioid antagonist, so it binds to opioid receptors and can reverse and block the effects of other opioids. It will restore normal respiration and eliminate the euphoria, or high, in a person who has suffered from an opioid overdose. The effects of naloxone, name brand Narcan, will generally last 30 to 90 minutes, if medical attention is not sought out, the overdose may return.
Upon using the opioid antagonist in the case of an overdose, the medication will almost immediately reverse the life-threatening suppression of breathing. Naloxone works by knocking off the opioid from the opioid receptor and then blocking the receptor. Because it blocks the opioid receptor naloxone cannot be abused nor cause overdoses.
Naloxone is administered two ways, as a nasal spray and as a liquid injection. Upon the medication being used, the patient may begin experiencing withdrawal symptoms which may be uncomfortable, but are not life-threatening. Some symptoms that they may experience include headache, changes in blood pressure, rapid heart rate, sweating, nausea, and vomiting.
Narcan has become more popular over recent years as opioid use and overdoses have risen. A few common opioids that naloxone can be used for include methadone, fentanyl, tramadol, heroin, oxycodone and hydrocodone. Recently, some lawmakers have made efforts to make Narcan’s availability more widespread. First responders have begun to carry naloxone to respond to and treat opioid overdoses.
Using Naloxone
CVS Pharmacies, which dispenses naloxone for those who need it, even without a prescription in most states, gave details on how to administer naloxone to help save a life.
The first thing to do when using naloxone is to identify the overdose. Opioids will suppress the body’s urge to breathe, so if you see that someone is struggling to breathe or is not breathing at all, call their name and rub your knuckles on their chest. If the person is unresponsive, they may be experiencing an overdose. Other signs include blue or pale skin, small pupils, slow heartbeats, snoring sounds, and gasping for breath.
The next step is to call 911. Naloxone only lasts for a short time, if emergency responders are not already on the way, it may be too late by the time they get there. If emergency services are not there in 30 to 90 minutes, the effects of naloxone may wear off and the individual could begin experiencing life-threatening problems once again.
The third step is to attempt CPR on the person overdosing. Be sure that nothing is blocking the person’s mouth that may impede breathing and place on hand on the person’s chin and tilt the head back. Pinch the nose closed and administer two slow breaths and look for the person’s chest to rise. Continue to give one breath every five seconds until the person begins breathing on their own. If the individual is still unresponsive after 30 seconds, it is time to use naloxone.
Follow the instructions for the type of naloxone you have, either inject in a muscle or spray into the nose. While your get ready, be sure to continue to give rescue breaths. After giving the person naloxone, continue to give rescue breaths. If the person remains unresponsive in two to three minutes, give another dose of naloxone and continue rescue breaths until emergency responders arrive.
You want to stay until help arrives to be sure that they don’t take more opioids and they don’t go back into an overdose and need more naloxone. The person may experience rapid or irregular heartbeats, chest pain, seizures, sudden stopping of the heart, or hallucinations. If they are feeling any of these tell emergency services immediately when they arrive.
Oklahoma and Naloxone
On average, one Oklahoman dies every day from an opioid overdose. An opioid overdose that can be prevented with the use of naloxone. In 2016, 54 percent of all overdose deaths in the state involved an opioid.
First responders across the state are recognizing the scope of the issue and the impact Narcan can have on it. From 2013 to 2016, the number of Narcan treatments used in the Tulsa metro area by emergency medical services nearly tripled.
Using an opioid blocker like naloxone to help users who have overdosed will not only save millions of dollars in hospital fees, it will also save the lives of thousands of people, something that can’t be measured with a dollar sign.
There has been legislative initiatives passed in recent years to try and make naloxone more readily available across the state as a preventative measure as a result of opioid addiction.
For instance, a law passed in 2017 that allowed for pharmacies and pharmacists to give out naloxone to anyone, not just people who had prescriptions. In fact, in 2017, all CVS pharmacies in Oklahoma made the overdose-reversal drug available without an individual prescription.
Other entities in the state have begun to recognize the need to make naloxone more available. Last year, The Oklahoma Sheriffs Association gave every Oklahoma sheriff and their deputies a supply of the medication, as well as training programs to ensure that the medication is administered properly.
More recently, Oklahoma state senator Greg McCortney introduced a bill, SB85, to the state legislature that would make it so that narcan would be available in public school should the need arise.
In a statement McCortney released after he introduce the bill, McCortney said, “It’s a proven fact that opiate antagonists can save lives,” said McCortney. “We just want to be certain that if school employees should need to administer this medication, they have the same legal protections given to others under state law.”
While most hope the naloxone would never have to be used on grade school students, the fact of the matter is that sometimes it is necessary. One recent example of this is when a 12-year-old girl at a Tulsa junior high school had to be taken to the hospital from school after a reported overdose. A spokeswoman for Tulsa Public Schools said that the student had ingested pills at her residence.
In a state with one of the highest prescribing rates in the country, a situation like this needs to be prepared for. With prescription pills so widely available throughout the state, it is easy for some students to get access to them through illicit sales or even just by raiding their parent’s cabinets.
Other Prevention Methods
Many see the use of naloxone as a harm reduction method. Harm reduction, while it does not endorse drug use, accepts the reality that people will use drugs and instead of focusing on prevention and punishment, focuses on reducing the harmful consequences associated with drug use. In the same way that condoms are now considered an effective form of prevention against pregnancy and disease transmission, harm reduction strategies for drug use aim to tackle problems like overdose deaths, HIV, crime, and incarceration.
One harm reduction strategy to reduce the risk of HIV transmission is to use needle exchange programs. People who inject drugs can substantially reduce the risk of getting diseases like HIV and hepatitis by using a sterile needle and syringe for each injection.
To some, the use of medication-assisted treatment (MAT) is considered a harm reduction method for dealing with addiction. Using methadone, a long-acting opiate, is one type of popular MATs that is used. The idea is that the addict will avoid withdrawal symptoms and the constant urges associated with it. Another advantage is that methadone is taken orally and controlled and gradually worked down in order to wean the patient off of opiates entirely.
One of the more controversial strategies to harm reduction is supervised injection sites. Popular in some countries, like Canada and Germany, a safe injection site allows drug users to go to a specific location where they recieve clean needles, a place to inject, and medical attention if the person overdoses. Despite the controversy of this method, there is some evidence that suggests that using safe injection sites is associated with 67 percent fewer ambulance calls and a decrease in HIV infections.
Reducing Stigma
There is a stigma surrounding drug users and drug use across the country, this is most likely a result of tough-on-crime laws and the drug war that were prevalent in the country in the 70s and 80s. The problem with this stigma is that it causes some users to not seek treatment due to the way they think they will be treated after admitting that they have an addiction. There are a number of educational and awareness campaigns that have begun in order to squash the stigma of addiction.
In Oklahoma there have been specific attempts to change the opinion surrounding addiction, and gain more support for people struggling with addiction. One example of this is OK I’m Ready, an educational website that aims to inform the public on the details of the opioid epidemic and how it is impacting Oklahoma specifically.
Prescription Laws
One of the best ways to cut down on opioid overdoses is to limit the number of opioids available to the population. Access to opioids is generally determined by the prescription rates of the drugs in the state. In 2012, Oklahoma had the fifth highest prescription rate in the country, with more than 127 prescriptions per 100 persons. While the number has declined over the past few years, they still have one of the top-10 highest rates in the United States.
One of the reasons for this decline is a number of laws that were made to create more oversight for prescriptions. Oklahoma first created opioid prescribing guidelines in 2013 and it was updated with additional materials in 2017. The guidelines included measures such as health care providers being required to seek out pharmacological therapies or non-opioid pain medications as the first option, opioids should not be prescribed for acute pain, and much more.
Similarly, the Oklahoma state legislature passed Senate Bill 1446. This law placed a limit on the number of opioid pills that physicians can prescribe. The law took effect in November of 2018 and made it so that physicians were not allow prescribe more than a week’s worth of opioid and must limit dosage to the lowest effective dose.
In Conclusion
There are a number of preventive methods that are being implemented in order to make progress on the opioid problem that takes tens of thousands of American lives every year. But, when the problem already exists in someone, substance abuse treatment is the best option forward. Landmark Recovery is dedicated to helping as many people as possible through our evidence-based treatment methods and our devoted staff and alumni network. Landmark can help you achieve and maintain sobriety. If you are interested in learning about our drug and alcohol rehab programs in Oklahoma City, please reach out to our admissions team today.

Choose Recovery Over Addiction
We're here 24/7 to help you get the care you need to live life on your terms, without drugs or alcohol. Talk to our recovery specialists today and learn about our integrated treatment programs.




