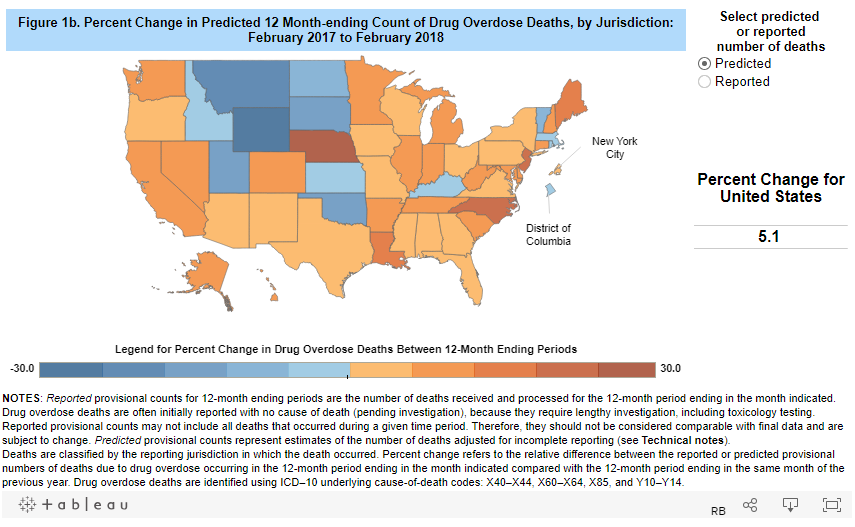
Substance abuse is one of the most pressing issues facing the state of Oklahoma. Within the past couple of decades, prescription painkillers, methamphetamine, and heroin abuse, as well as deaths from overdose have all steadily increased year over year. In 2017, overdose deaths throughout the United States jumped 10%, reaching roughly 72,000, according to the Centers for Disease Control and Prevention. According to data from the Mental Health and Substance Abuse Services Department of Oklahoma, the state has some of the highest rates for mental illness and substance use disorders.
In 2017, Oklahoma reported the highest number of individuals using prescription painkillers for non-medical purposes, at a rate of 5.31%, with Minnesota reporting the lowest at 3.41%. In the last 15 years, deaths from overdose have increased by 91%, and annually the state loses nearly 1,000 people to overdose on average. Addiction has spurred a rise in incarceration rates, with families being ripped apart and billions lost in workplace productivity. Lawsuits are also piling up in Oklahoma and around the country targeted at holding pharmaceutical giants responsible for offloading massive quantities of opioids and downplaying the severe addictive qualities they contain.
In 2017, Mike Hunter, Attorney General for Oklahoma, joined a coalition of lawsuits aimed at opioid manufacturers such as Purdue Pharma LP, Teva Pharmaceuticals, Johnson and Johnson. Filed on behalf of the state of Oklahoma. This lawsuit accuses the giant pharmaceutical companies of recklessly distributing opioid medication and engendering a false community belief in the safety and efficacy of opioid medication for treating pain. The companies also stand accused of intentionally misleading doctors and the public; an accusation backed up the by the existence of numerous internal memos and correspondence referencing the street price of drugs such as Oxycontin and its addictive qualities.
The Commission on Opioid Abuse
By joining more than 600 state and local governments in filing suits against big pharma, Oklahoma continues to push back against addiction and lead the good fight. The Oklahoma Senate followed up on this lawsuit by creating the Commission on Opioid Abuse, a state-funded coalition tasked with researching and proposing solutions for curbing the growing prevalence of addiction. By drawing wisdom from members of the medical community, law enforcement, and business owners, this 9-person committee has already made progress in the fight against addiction, reversing the trend of overdoses while the country average continues to climb.
According to the Oklahoma State Department of Health, there were more than 750 unintentional drug poisoning deaths in the state in 2016, with more than half attributable to prescription medication mishandling. Between 2012 and 2016 in the state, more than two-thirds of drug overdoses were related to prescription drugs, with 64% involving opioid-based painkillers.
Why Oklahoma?
Oklahoma has only been one of many states affected by the way opioid manufacturers distributed their product. Multi-pronged marketing campaigns were dispersed nationwide and aimed at downplaying the danger of opioids, touting pain as “the fifth vital sign” that clinicians needed to address in order to serve their patients adequately. Manufacturers also recruited the help of doctors in pushing for new Pain Management Standards that would allow them to prescribe opioid painkillers more freely. In 2001, the Joint Commission did just that, by beginning to require doctors to ask patients about their pain. The first decade of the 21st century saw global consumption of opioids increase by 250%.
In 2014, Oklahoma was ranked the number one state in the U.S. for the number of individuals hooked on painkiller medication. In 2016, a record number of Oklahoman’s, 952, died from drug overdose, with methamphetamine being the largest culprit. The three most prevalent drugs were methamphetamine, opioids, and heroin, accounting for more than 95% of overdose deaths. Kevin McIntire, who leads a drug task force in Oklahoma, compares the sizes of meth labs between then and now: “There is no comparison to the amount of buying power and capital that Walmart has to local mom-and-pop shops. It’s the same thing as the cartels – the financial backing, the hierarchy. You can’t compare a local methamphetamine cook to that.” In 2016, the state lost almost one person per day to meth overdose, losing an estimated 333 people. The total death count was more than other drugs such as oxycodone, hydrocodone, and heroin combined.
The culprit behind this rise in methamphetamine overdoses? Mexican drug cartels that are producing the purest and most potent meth seen in decades in super labs spread throughout Mexico. From Oklahoma all the way to Southern California, law enforcement are designating meth as the biggest threat they are currently facing. Beyond the excessive violence and associated criminal activity of methamphetamine, there is also the lack of available medication to treat withdrawals. For heroin and other painkillers, medications such as Suboxone, methadone, and buprenorphine can relieve a person’s cravings as they detox from chemical dependency. However, there is no such medication for methamphetamine. Experts believe that it can take up to three years for someone to feel healthy and happy again after giving up methamphetamine.
HIV Outbreak in Oklahoma
The CDC has identified both Jefferson County and Cimarron County with Oklahoma as a county at risk for an outbreak of HIV or Hepatitis C. Drug-related deaths within the state have increased at a similar rate to the United States average but remain slightly higher. However, inpatient stays due to opioid abuse have remained level, indicating that there may be a lack of adequate access to these kinds of resources. Drug and alcohol rehab in Oklahoma are essential to combat the rising crisis of opioid and other drug addictions within the state.
- In 2016, there were 444 deaths directly from opioid overdose, equal to a rate of 11.6 deaths per 100,000.
- Heroin deaths within the state more than doubled from 2015-2016.
- In 2015, Oklahoma clinicians wrote 101.7 opioid prescriptions per 100 people totaling nearly 4 million opioid prescriptions for the year. This is 30 more per person than the national average.
- Oklahoma’s incidence of HIV cases related to intravenous drug use is almost twice the national average.
Mike Hunter, Oklahoma Attorney General, commended a new initiative created by Walmart to help safely dispose of excess medication. The method of disposal utilizes a special powder that it is mixed with water and allows users to dissolve their pills safely. The brand name, DisposeRx, is going to be carried in all Walmart pharmacies starting in 2018, some 4700 stores nationwide. The substance is a powder that is mixed with warm water within the container, creating a special gel that solidifies and disables the chemical compounds.
Due to the high amount of opioid abusers who start out taking the medication from a friend’s or relative’s medicine cabinet, this method could be an effective way to cut down on prescription medication abuse significantly. Said Attorney General Mike Hunter:
“The pioneering initiative from a corporate partner like Walmart is a positive step in the battle against the opioid epidemic. It is reported that more than two out of three individuals who misuse opioids get them from a medicine cabinet and approximately 80 percent of heroin users abused prescription painkillers first. This is a simple solution to the growing problem of unused prescription pain medication left in the household.”
To adequately address the nation’s rising crisis of deaths relating to suicide, alcohol, and drug use will require a comprehensive treatment approach that involves health care systems, communities, and businesses to rally and face the problem head-on.
States Battling Against Addiction
As the national average slowly climbs upwards, several states, including Hawaii, Massachusetts, North Dakota, Oklahoma, Rhode Island, Utah, Vermont, and Wyoming have all managed to reverse the trend of drug addiction, reducing the number of overdose deaths. These states have been at the forefront of the fight against addiction, implementing multiple approaches that are showing promising results. These include increasing access to the anti-overdose medicine Naloxone, increasing access to tapering medications such as buprenorphine and methadone, and doing a better job tracking the flow of drugs between doctors and patients.
Insurance Coverage
One of the reasons that these locations have seen success can be attributed to boosting the number of insured individuals within the state. People with substance use disorder are also likelier to suffer from mental illness and to struggle financially as a result of their addiction. Without health coverage, treatment can remain unattainable for many. In states like Massachusetts and Vermont, legislators have expanded access to Medicaid under the Affordable Care Act and encouraged more participation with private insurance. In 2016, 2.5% of people in Massachusetts and 3.7% of people in Vermont lacked insurance, compared to 8.6% for the country as a whole.
For individuals within these two states, more than 60% of people with an opioid use disorder are receiving medication-assisted treatment, according to a Blue Cross Blue Shield Association report. This in contrast to states like Florida, Georgia, and Texas where Medicaid remains tightly bound, the uninsured rate is more than 12%, and less than 30% of people with opioid use disorder are receiving medication-assisted treatment. As Trump and the Republican House work to dismantle what remains of the Affordable Care Act, many addicts will be left unable to afford the treatment they desperately need.
Medication Assisted Treatment
Access to health insurance is essential, but making sure that local healthcare options provide adequate treatment is even more vital. The partial opioid agonist Suboxone has been linked to reducing overdose deaths in France by nearly 80%, but lawmakers and health officials are hesitant to spend public tax dollars on any form of treatment that looks like swapping one drug for another. In Vermont, policymakers have used state funds and federal grants to hire nurses and social workers that can follow up regularly with patients taking Suboxone and make sure they are getting back on their feet.
The Vermont Department of Health conducted a study on their follow up programs to determine how effective they could be in curbing opioid usage. The results were astounding, with 96% of patients decreasing opioid usage and an 89% reduction in emergency department visits, as well as a 90% reduction in illegal activity. Massachusetts has also found success in providing state funding for follow up personnel for those leaving rehab. They have also upgraded state-level prescription drug monitoring to make sure that doctors aren’t over-prescribing pain medications. Since 2016, opioid prescriptions have dropped by 30%.
Tackling the Epidemic as a Whole
Rhode Island has addressed part of the drug problem by expanding access to treatment in state prisons. Globally, there is no more high-risk period and population than those leaving incarceration. Although the program is still relatively new, a recent study has found that overdose deaths among released inmates have been reduced by more than half. In San Francisco, city health workers are offering treatment to addicts who are homeless, planning to spend more than $6 million on the program within the next two years. Members of the team travel around the city offering buprenorphine prescriptions to homeless addicts which they can fill the same day.
Facing Addiction
One advocacy group that is pushing the country to create much-needed change in the realm of addiction treatment is Facing Addiction. This organization is partnered with the health care consulting firm Leavitt Partners, which has gathered experts and industry leaders together to promote new care models that emphasize long-term recovery using evidence-based practices. Another organization, Shatterproof, is a collective that works with over 16 health insurers in adopting universal screening, access to medications, and regular outpatient care. The idea is that once private insurers can recognize these standards and create financial incentives for health care systems to meet them, we can begin to offer more affordable treatment to those who need it.
In Conclusion
These efforts demonstrate what it would look like for the nation to start treating addiction in for the epidemic that it indeed is. The government used similar tactics to fight back against the AIDS epidemic of the 1980’s, but lawmakers in Congress have not pledged to fight against this growing scourge with the same kind of united front. By examining the breakdown of states by overdose rates, we can see that several areas have been successful in reversing the national trend. The Midwest remains the most devastated by addiction, but states such as West Virginia and Oklahoma demonstrate the effects of a concerted effort.

Choose Recovery Over Addiction
We're here 24/7 to help you get the care you need to live life on your terms, without drugs or alcohol. Talk to our recovery specialists today and learn about our integrated treatment programs.