Narcan can save the life of someone overdosing on opioids
About every 12 minutes someone overdoses on opioids without Narcan around to stop the overdose. These overdoses can happen at any time and can even occur when opioids are used as directed. What would you do if you saw someone overdosing on opioids? Would you know how to help them?
There’s a nationwide push to make the life-saving drug Narcan more accessible. Narcan, the brand name of a medication called naloxone hydrochloride, can stop or even reverse the effects of an opioid overdose. It’s also used in medication-assisted treatment to assist the recovery of those suffering from an opioid use disorder. Narcan is the first federally approved nasal spray form of naloxone.
Narcan was developed off the back of research funded by National Institute on Drug Abuse (NIDA) back in 2015. By 2019, a generic naloxone nasal spray was also approved by the FDA giving consumers more market choice. A Narcan sprayer requires no assembly, and the drug is sprayed into one nostril while patients lay on their back. Once Narcan is used on a patient who is going through an opioid overdose, it will reverse the sedative effects of the drug and restore the individual to a natural breathing rhythm. Naloxone is now available in three FDA-approved formulations including Narcan:
- Injectable
- Auto-injectable
- Nasal Spray

Our handy guide to Narcan
What’s an Opioid Antagonist?
Naloxone hydrochloride is an opioid antagonist designed to rapidly reverse and stop the life-threatening effects of an opioid overdose. An opioid antagonist means that it will bind to opioid receptors in the brain and reverse or block the effects of other opioids. Common examples of opioids include morphine, codeine, oxycodone, hydrocodone, fentanyl and heroin. It will quickly restore normal respiration to a person whose breathing rate has slowed or stopped because of overdosing on opioids. The medicine can also reverse the sedative effects and unconsciousness that are common during opioid overdoses.
Is Narcan Safe?
The medicine is non-habit-forming and has virtually no effect on people who are not overdosing. Naloxone is an extremely safe medication that only has a noticeable effect on individuals who have opioids in their system. Individuals who receive Narcan for an overdose should be observed constantly until emergency care services arrive and be medically supervised for at least two hours after the medication is administered. According to former U.S. Surgeon General Jerome Adams, naloxone is effective at reversing the effects of an opioid overdose.
Adams stated, “Expanding the awareness and availability of this medication is a key part of the public health response to the opioid epidemic. Naloxone is a safe antidote to a suspected overdose and, when given the time, can save a life.”
It should be noted that there are several side effects associated with Narcan and naloxone. Some people will even experience sudden opioid withdrawal symptoms. Some of these symptoms include:
- Body aches
- Diarrhea
- Increased heart rate
- Runny nose
- Fever
- Sneezing
- Sweating
- Yawning
- Nausea
- Vomiting
- Restlessness
First Generic Nasal Spray for Opioid Overdose
On April 19, 2019, the FDA approved the first generic naloxone nasal spray to treat opioid overdose. The FDA press release surrounding the approval states:
“In the wake of the opioid crisis, several efforts are underway to make this emergency overdose reversal treatment more readily available and more accessible. In addition to the approval of the first generic naloxone nasal spray, moving forward we will prioritize our review of generic drug applications for naloxone.”
The FDA also expressed its intent to promote competition and reduce drug prices by improving access to safe and effective generic medicines for all types of ailments. The new generic naloxone nasal spray was developed by Teva Pharmaceuticals and received initial approval in June 2018.
The Growing Demand for Narcan
When used in hospitals, naloxone is normally administered via an IV line or intramuscular shot. Since the medication can also be absorbed into the bloodstream by nose, some medical technicians started fitting the IV formulation with a makeshift adapter to atomize the naloxone, allowing it to be sprayed into the nose. From the hospital, where it’s often already too late to revive someone, to police officers and firefighters, Narcan is now more widely used. With the death toll from the opioid crisis mounting, increased access to Narcan has become a pressing concern.
It makes sense for the antidote to make its way into the hands of first responders since the effects of opioid overdose can kick in so quickly, but many of those who have even quicker access to the victims of an overdose became concerned with their own access to such a successfully lifesaving drug.
A seminal 2013 study showed a correlation between improved overdose education and the distribution of nasal naloxone in communities blighted by the opioid epidemic. Sadly, increased demand for naloxone saw the price ratchet up in the form of the Narcan nasal spray ($150 for a 2-pack) and the Evzio auto-injector (an eye-watering $4500). Both solutions were vigorously criticized for these sky-high list prices. As a result, generic nasal spray naloxone is much cheaper than the brand-name alternative, making it readily available to those who may be able to save someone’s life.
Identifying an Opioid Overdose Emergency
Overdoses happen when the body has been overloaded with a medication or illicit drug. Because they affect the part of the brain that controls breathing, if opioid levels are too high it can cause breathing to slow down to dangerous levels and can even result in death.
Common signs and symptoms of opioid overdose include:
- Unusual sleepiness or unresponsiveness
- Slow breathing
- Slow heartbeat
- Cold or clammy skin
- Tiny pupils
- Blue lips and nails
Some people are at a higher risk than others for opioid overdoses. For example, those taking higher doses or those taking opioids in combination with other medications or alcohol are at a much higher risk of overdose. Others who may also be at higher risk include:
- People with medication conditions like depression or HIV
- Household members of people in possession of opioids
- Those with a history of substance abuse
- People with reduced tolerance following detoxification or incarceration
How to Administer Narcan
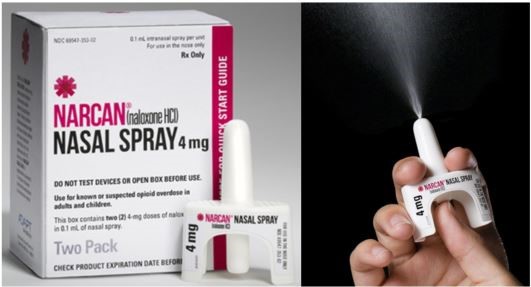
Narcan was developed to be used at home without the need for medical training. If you suspect that someone has overdosed on opioids, you may need to administer Narcan. To administer Narcan, remove the packaging for the device and hold it with your thumb on the bottom the plunger and two fingers on the nozzle. Then, place and hold the tip of the nozzle in either nostril and press the plunger to release the dose into the patient’s nose. If breathing does not return to normal after two to three minutes, give the person an additional dose of Narcan in the other nostril using a new device.
It should be noted that Narcan is not a substitute for medical care and that you should always call 911 as soon as possible, even if the person wakes up and becomes conscious again.
CVS Pharmacies has a guide for responding to an overdose with Narcan on its website:
- Identify the Overdose — Opioids will suppress the body’s breathing rate. If you notice this, try calling the person’s name or rubbing your knuckles on their chest. If there is no response, the person may be experiencing an overdose.
- Call 911 — It is important to get professional help as soon as possible. Make sure to call 9-1-1 and give a clear address and location. Tell the operator that the person is unresponsive and not breathing or having difficulty breathing.
- Give Rescue Breaths — Giving a person who is experiencing an overdose basic CPR can be an effective way to deal with the situation. Be sure that nothing is in the person’s mouth that is blocking breathing, place one hand on the person’s chin, and tilt the head back. Pinch their nose, administer two slow breaths, and look for the person’s chest to rise.
- Give Naloxone — It is best to follow the specific instructions set out on the form of naloxone that you have. Following the administration of naloxone, continue to give rescue breaths at a rate of one breath every five seconds.
- Wait for Help — Stay with the person, even if their breathing returns to normal. Wait until paramedics arrive.
Where Can I Get Naloxone?
Until the last decade, naloxone was generally only available with a doctor’s prescription. However, as of March 2019, all states and territories within the US allow those who wish to obtain some form of Narcan without a prescription to legally obtain it. Between 2010 and 2014, the number of local sites providing naloxone more than tripled and there were more than two-and-a-half times the number of overdose reversals reported.
Generally, doctors write blanket prescriptions for pharmacies. By doing this, pharmacies can provide Narcan/naloxone to anyone who comes in to ask for it. Similarly, Narcan is covered under most insurance plans.
Can Narcan Be Abused?
Narcan does not have abuse potential. Narcan is a life-saving drug. Opioids cause euphoric and sedative highs; if Narcan is used the drug will reverse that high and stop the effects of the opioid drug which, sometimes, will put a person in a state of withdrawal. These withdrawal problems will be uncomfortable but will not be life-threatening. The benefits of using Narcan or naloxone greatly outweigh the potential consequences. It is not possible to overdose on Narcan and if someone were to take it with no opioids in their system, it would have no effect at all.
Side Effects of Narcan
Narcan is extremely safe with a noticeable effect only on someone with opioids in their system. While naloxone can cause mild withdrawal symptoms, these symptoms are negligible compared to the consequences of an opioid use disorder.
In the worst scenario, using Narcan can cause:
- Changes in blood pressure
- Headaches
- Nausea
- Sweating
- Tremors
- Vomiting
Someone who has been using opioids regularly might experience sudden opioid withdrawal symptoms after a spray of Narcan. These symptoms can include:
- Aching body
- Diarrhea
- Fever
- Goose bumps
- High blood pressure
- Increased heart rate
- Nausea and vomiting
- Nervousness
- Restlessness
- Runny nose
- Shivering
- Sneezing
- Stomach cramps
- Sweating
- Yawning
- Weakness
Once you’ve administered Narcan, you should closely observe the person until medical help arrives. Inform medical personnel of the timing of the last dose of Narcan. The person will need to be monitored for at least 2 hours after that.
Remember: Narcan will have no negative effects unless someone has opioids in their system. If you’re at all concerned about the side effects, they are non-issues compared to the real risk of death from opioid overdose.
Narcan Statistics
Narcan is effective. It will quickly restore a person’s breathing to normal and can save their life. Case studies have shown just how effective it can be.
A naloxone distribution program in Massachusetts was effective in reducing opioid overdoses by 11%. From 1996 to 2014, at least 26,500 opioid overdoses in the United States were reversed using naloxone. Just in 2017 alone, there were over 70,000 drug overdose deaths in the country. This means that more Americans died in one year due to drugs than during the Vietnam War. If you take a step back and look at overdose deaths over the past 18 years, you will find that more died from the drug epidemic than in World War I, The Vietnam War, and the Korean War combined.
As the opioid crisis has grown, so has Narcan and naloxone administrations. While there is still more work to be done to make this medicine more widely available, it has still helped save the lives of thousands of individuals.
The Future of Overdose Protection Solutions
The NIDA is continuing to funnel funding into the development of overdose-reversal medications with the potential for longer action. This is especially valuable where powerful synthetic opioids like fentanyl are involved.
Researchers looking into longer-action opioid antagonists are focusing on an intra-nasal version of nalmefene which already comes FDA-approved in injectable form. Methocinnamox (MCAM) is another substance showing promise for longer-acting reversal.
Research has also shown a wearable device might have promise. This device automatically administers a large dose of naloxone if overdose-induced respiratory failure is detected. This is achieved in line with a smartphone app that shows promise in identifying breathing problems and other factors linked to acute opioid toxicity. The future is promising for these early warning systems and overdose-reversal agents.
Treatment
For opioid addiction treatment, it’s best to seek out the help of a rehab facility. Drug and alcohol treatment centers can offer patients access to treatment that specifically helps patients safely deal with the side effects and withdrawal symptoms associated with short-term sobriety. Following detox, patients will go through individual and group therapy sessions as they learn more about addiction and how to prevent relapses.
Following discharge from a residential facility, many patients choose to continue treatment through an outpatient treatment program that helps them continue down their path of last8ing recovery as they adjust to a new lifestyle.
Treatment is an option that should be taken very seriously when you or your loved one suffers from an opioid overdose. Treatment, while not always successful on the first try, can help open someone’s eyes to the damage that is being done through opioid abuse.
Getting Help for Opioid Addiction
Narcan and naloxone can be life-saving medicine. It can be used to reverse an opioid overdose and restore someone’s breathing back to normal. While problems can arise following the administration of naloxone, such as the onset of withdrawal symptoms, these are nothing compared to the life-threatening consequences of an overdose. Surviving an overdose can be a traumatic experience and some will look to start living a life in recovery after this happens. However, many will not know where to begin.
Landmark Recovery is a drug and alcohol treatment center that is dedicated to helping as many people as possible and save one million lives in the next century. If you’re interested in learning more about a personalized treatment plan, please visit our website and reach out to our admissions staff today at 888-448-0302.

Choose Recovery Over Addiction
We're here 24/7 to help you get the care you need to live life on your terms, without drugs or alcohol. Talk to our recovery specialists today and learn about our integrated treatment programs.



